
A comparison of ophthalmic education in China and America
Introduction
Ophthalmology was among the western medical specialties first introduced to China in the 1800s (1,2). Western medicine is quite different from traditional Chinese medicine but the new ophthalmic knowledge and techniques were gradually accepted and widely spread across the country through the great efforts of Chinese medical educators. Keeping pace with the fast development of the field and training qualified ophthalmic professionals is always a vital aim for medical education but also poses a huge challenge for large countries. This perspective compares the current ophthalmic education system in China and America. The training system in the US is relatively mature with national accreditation standards, while China is moving rapidly towards consistent nationwide subspecialty training and introducing innovative training reforms. We hope this analysis will provide useful details about both ophthalmic education programs to help improve the training designs and curriculum.
Ophthalmic education in America
The US ophthalmic education system strives to meet the comprehensive standards (requirements) to train MDs who provide equal quality of general and subspecialty eye care services nationwide. These standards are set in the context of supervision by qualified faculty to prepare resident and fellow physicians with the skills, knowledge, and attitude to take personal responsibility to provide the highest quality care of individual patients.
Ophthalmology residency
Ophthalmology residency is the fundamental 4-year training that is well structured and standardized by the Accreditation Council for Graduate Medical Education (ACGME). There are about 116 residency programs meeting the rules of the ACGME to ensure training in all subspecialties to prepare a competent general ophthalmologist. Residency graduates are expected to have a solid broad foundation of knowledge, to master the common management protocols, and to be comfortable performing general ophthalmology procedures with an emphasis on phacoemulsification. Each year, about 800 US medical school seniors who want to be an ophthalmologist compete for about 590 training positions. After a year of general medicine internship (PGY-1), residents undergo a 3-year ophthalmology residency training (PGY2–4). During this time, the residents will rotate through all subspecialties and complete at least a minimum number, oftentimes much more, of procedures in each subspecialty as primary surgeon with supervision. Besides clinical training, residency programs provide supplemental didactic activities including Basic and Clinical Science Course (BCSC) lectures, grand rounds, surgical wetlabs, journal clubs and conferences. Involvement in research is always encouraged. The annual in-service exam (OKAP) is mandatory for every resident and provides a percentile rank score among the same training class nationwide. The ACGME committee oversees regular resident milestone reports, training case/rotation/duty hours/didactic logs, formal two-way evaluation on every rotation, yearly faculty and trainee detailed program surveys and administrative re-qualification assessment every 5 years. Training institutions are famous for their academic reputation, cutting edge research, strength of faculty, and thoroughness of patient care including very complex cases. Patients in resident clinic are fully aware that they are under the care of the doctors in-training with attending’s supervision. Excellent patient rapport eases resident-patient communication and institutional reputation assists the training program.
Continuing medical education (CME) after residency
CME after residency is mandatory for licensure and tracked by the American Board of Ophthalmology (ABO). New residency graduates are labeled board-eligible ophthalmologists until they become board-certified after passing the written qualifying exam and oral examination. The average written exam passing rate is around 72–75% while the oral exam is an in-person, timed patient management problem interview, which has a pass rate around 75–86%. Re-certification is required every 10 years, a process called maintenance of certification (MOC) which includes a quality improvement activity. Board review courses are available all year around. Besides knowledge assessment, lifelong learning is promoted by requiring 25 hours of CME credits including 2 hours of ethics training yearly for every practicing ophthalmologist.
Subspecialty fellowship training
About 65% of the graduating ophthalmologists choose to undergo additional 1–2 years subspecialty fellowship training to be more comfortable with managing advanced, complex and unusual cases in glaucoma, medical or surgical retina, cornea, oculoplastic, pediatrics, and neuro-ophthalmology. Fellowship training is another well-standardized training program monitored by the subspecialty society similar to how ACGME monitors residency training. The fellows shadow the preceptors in their faculty practice, act independently seeing patients, and perform primary procedures or assist in the operating room under supervision. In some academic programs, fellows run the subspecialty management with much more autonomy. They are responsible for the complete management of the patient, and attending preceptors serve only as an onsite consultant. During surgery, attendings scrub-in with the fellow guiding them until they are able to perform the procedure independently. In the later stage of training, most fellows will staff residents in subspecialty clinics, following the classic mantra of “see one, do one, teach one.” Some fellows also teach residents in the OR at medical school teaching hospitals. In private academic programs, the supervision is often tighter as patients expect the attending to be the primary surgeon. Fellows still gain experience by shadowing the preceptors and have hands-on supervision in OR with more select cases.
Physician scientist training
About 10% ophthalmologists are interested in a career as a physician scientist. Some have PhD training and enjoy bench lab or basic science fundamental or translational research. Others are more interested in clinical studies. The latter may choose to add a 1-year research fellowship in addition to clinical training or pursue a master’s of public health. Research fellowships are similar to postdoctoral training but can vary a lot based on the individual institute.
Learning resource
Along with a strong ophthalmic education foundation, most American ophthalmologists have ample resources to keep their knowledge and procedural techniques up-to-date. The annual American Academy of Ophthalmology (AAO) national society conference and subspecialty society conferences are easily accessible to all AAO and subspecialty society members. Each subspecialty also has an internet-based forum as an excellent platform for members to share experiences and challenging cases. Second opinions for complex cases frequently receive instant comments which benefit both the subject presenter and the thread followers. US-based eyecare companies are always striving to promote new medications and equipment. Thus, they consistently support relevant educational lectures and conferences. Wetlabs and demo equipment are easy to request. A well-trained technical company representative is usually involved in the first five procedures when an ophthalmologist is trying out new equipment and techniques. There are strict regulations governing the interactions between physicians and industry to minimize conflicts of interest.
Ophthalmic education in China
China is among the most populous nations in the world with approximately 1.4 billion people distributed over 23 provinces, 5 autonomous regions, 2 special administrative regions and 4 metropolitan municipalities. Problems such as inequality in access to health resources and inefficiency of medical care delivery exist. In order to meet the tremendous healthcare demands relative to the limit number of trained physicians and to reduce geographic disparity of health care services, the medical education system in China has been evolving dramatically over the past few decades, and the Chinese ophthalmic education system constantly strives to improve the quality of its specialty.
General information about Chinese medical education
In contrast with the US, Chinese students choose clinical medicine as their major upon graduation from high school. Currently, China has 268 medical schools, producing 144,000 graduates per year (3). The MD degree programs are complex and consist of varying durations lasting from 5 to 8 years. Although several apparent structural and operational differences in the medical training systems exist between the two countries (Table 1), the clinical training processes one specialist (such as an ophthalmologist) must go through are quite identical. In China, this process includes the undergraduate combined medical education, specialty training (residency) and subspecialty training (fellowship); the latter two are also known as postgraduate education program.
Table 1
| Variables | China | US |
|---|---|---|
| Students enrolled | High school graduates | Bachelors |
| Students amount | Huge | Small |
| Length of schooling | Varied | Regular |
| Academic degree | MD | MD (bachelor, Master, Doctor) |
| Evaluation | Nationwide examination | Nationwide examination combined with interviews conducted by training institute |
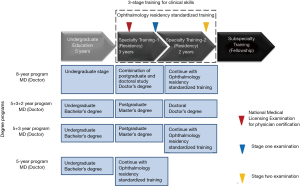
Figure 1 described four typical pathways that Chinese medical students went through to get accredited as an ophthalmologist. Clinical doctors must first complete the undergraduate curriculum, normally 5 years, with emphasis on basic biomedicine, medical technology and clinical medicine. The curriculum also includes content covering humanities, ethics, and public health. After the undergraduate program, medical students may choose ophthalmology as their specialty. They then will complete 5 years of residency training (3 years for the first stage and 2 years for the second stage). After that, some may continue to receive extended training in a subspecialty. Meanwhile, young doctors are eligible to take the National Medical Licensing Examination for physician certification after complete the second years of residency. This examination is conducted by the National Medical Examination Center. After passing, one will be approved by registering with the National Health and Family Planning Commission of the People’s Republic of China before practicing medicine as an independent physician.
Standardized ophthalmology residency training
Standardized ophthalmology residency training is now implemented nationwide and is considered as the fundamental part of the Chinese ophthalmic continuing education program (4,5). Estimated 100 residents per city were enrolled in this program. The program is designed in two stages as mentioned above. The requirements were published by the former Ministry of Health in 1993. The rapid expansion of residency trainees yet lack of surgical training cases, inconsistency of medical school education backgrounds and relative scarcity of educational resources and free time among faculty educators have combined to pose great challenges towards achieving standardized nationwide ophthalmic residency training programs across China. To ensure equal resident education, most of the ophthalmic training institutes are university-affiliated hospitals with certification from a supervision agency. The teaching capacity of the training base is re-assessed every year. Participants applying for ophthalmic training positions are required to pass the interviews conducted by training institute. During rotations, residents are provided opportunities to perform certain procedures with guidance from supervisors. They are expected to become proficient with general ophthalmology techniques in addition to a fundamental foundation of ophthalmic knowledge. Training requirement for each subspecialty is contained in documents officially published by the former Chinese Ministry of Health. Residents are evaluated after each subspecialty rotation. The scores are recorded and reported to the supervision agency. Every resident is encouraged to participate in at least one scientific research and is assigned a mentor. They also have full access to lectures and forums about ophthalmology and other specialties to keep pace with new knowledge.
Mandatory CME credits are required for graduation. After 3-year first stage training, residents will take the written and oral examinations held by Municipal Commission of Health and Family Planning to obtain the certification (Stage one examination). Then they can move on to the second stage of training which includes opportunities as chief resident and participating in independent patient management, teaching and administrative activities. Residency training and passing stage two examination are the prerequisite for promotion to attending. Detailed comparison between China and US regarding ophthalmic residency training is listed in Table 2.
Table 2
| Variables | China | US |
|---|---|---|
| Training length (years) | 5 | 4 |
| Stages | First stage (3 years) | PGY-1 (1 year) |
| Second stage (2 years) | PGY2ñ4 (3 years) | |
| Training position each year | Estimated 100/city | 590 across the country |
| Training content | Subspecialty rotation | Subspecialty rotation |
| Scientific research | Scientific research | |
| Lectures and forums | Basic and Clinical Science Course (BCSC) lectures; grand rounds; surgical wetlabs; journal clubs; conferences | |
| Requirement of outpatient visits for each resident | About 2,200/year | About 1,000/year |
| Evaluations | Exams held by training institute after each rotation | Annual in-service exam (OKAP) |
| Stage one examination held by Municipal Commission of Health and Family Planning | Regular resident milestone reports, training case/rotation/duty hours/didactic logs, formal two-way evaluation on every rotation, yearly faculty and trainee detailed program surveys supervised by ACGME | |
| Training center administrative re-qualification assessment | Every year | Every 5 years |
Continuing education programs and subspecialty training
Continuing education programs provide mandatory courses after residency. Twenty-five hours of CME credits are required each year. Subspecialty training is mainly organized by hospitals which have outstanding strength in the corresponding fields. Subspecialty training curriculums are set by individual institutes. Besides those well standardized programs, many learning resources are also available for Chinese ophthalmologists (6). Annual meetings of the Chinese Ophthalmology Society and conferences for subspecialty societies are held regularly. More and more international ophthalmological conferences are organized in Chinese major metropolitans. Foreign experts frequently attend these conferences as speakers and program modulators, that provides direct communication with all level of the Chinese ophthalmologists. Internet-based forums for educational topics, lecture series and interesting cases are boosted fast. Wet-labs for surgery skills become more available through the institute and eye care companies.
Huge patient volume is a heavy load for every level of the Chinese eye care system, it is also a good resource for the young ophthalmologist to get matured in their knowledge and skills. A trainee will see average 2,200 patients per year. Stage two residents compete for the chances participating in the charity surgical eye care such as Lifeline Express. Performing 300 cataract extractions in 3 months granted them a much advanced surgical skills.
Conclusions
China has a different ophthalmic training paradigm from the US. Great efforts have been exerted by the government and all eye care providers to reach higher medical levels and provide the most advanced service for Chinese patients.
Acknowledgments
Funding: None.
Footnote
Provenance and Peer Review: This article was commissioned by the Guest Editors (Karl C. Golnik, Dan Liang and Danying Zheng) for the series “Medical Education for Ophthalmology Training” published in Annals of Eye Science. The article has undergone external peer review.
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aes.2017.06.12). The series “Medical Education for Ophthalmology Training” was commissioned by the editorial office without any funding or sponsorship. The authors have no other conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Liu X. Western medical education in Guangdong Province in modern China. Zhonghua Yi Shi Za Zhi 1986;16:148-51. [PubMed]
- Lu P. Modern woman medical education in China after the introduction of western medicine. Zhonghua Yi Shi Za Zhi 1999;29:42-5. [PubMed]
- Lv X, He H, Wu Z. China's Medical Education and Interventional Neuroradiology Training. World Neurosurg 2015;84:1462-5. [Crossref] [PubMed]
- Xiao YT, Wang YT. Standardised residency training: students' concerns. Lancet 2017;389:905. [Crossref] [PubMed]
- Zhu J, Li W, Chen L. Doctors in China: improving quality through modernisation of residency education. Lancet 2016;388:1922-9. [Crossref] [PubMed]
- Tso MO, Goldberg MF, Lee AG, et al. An international strategic plan to preserve and restore vision: four curricula of ophthalmic education. Am J Ophthalmol 2007;143:859-65. [Crossref] [PubMed]
Cite this article as: Liu Z, Liu M, Chang R, Huang P, Zhang C. A comparison of ophthalmic education in China and America. Ann Eye Sci 2017;2:35.


