
Iridofundal colobomas may lower severity of retinopathy of prematurity
Introduction
Iridofundal coloboma (IFC) is a defect along the length of the choroidal fissure that failed to close during embryogenesis (1). Normal closure of the fissure occurs between 5th and 7th week of fetal life, and the defect may involve iris, ciliary body, zonules, retina, choroid and optic disc (2). Associated ocular abnormalities with IFC are present in nearly 15% of the cases; however retinopathy of prematurity (ROP) has not been reported thus far (3). Herein, we report the first case where unilateral IFC was observed with asymmetric ROP.
Case presentation
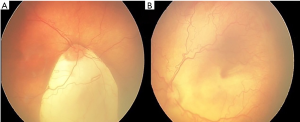
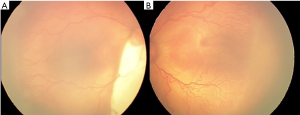
A male baby, second child of a twin pregnancy delivered by cesarean section at 28 weeks of gestation, was referred to us at 38 weeks post conceptional age for ROP screening. The child had history of respiratory distress syndrome for which he had received surfactant therapy along with supplemental oxygen for 30 days and assisted ventilation support for 10 days. The child had received blood transfusion in view of anemia and low hematocrit. Anterior segment examination revealed iris coloboma in right eye, with no other related ocular abnormalities like micro cornea, microphthalmos, and lens opacity. Fundus examination of right eye revealed type 2 choroidal coloboma (Ida Mann Classification System)(Figure 1A), with stage 2 ROP in zone 3 and no plus disease (Figure 1B). The left eye fundus revealed no choroidal coloboma (Figure 2A) with stage 3 ROP in zone 2 with plus disease (Figure 2B). The child was evaluated for anomalies commonly associated with IFC, like congenital heart defects, choanal atresia and ear anomalies but no systemic abnormality was found.
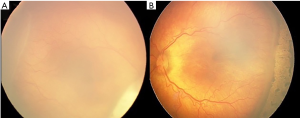
As per the recommendations of the Early Treatment for Retinopathy of Prematurity (ETROP) study (4), immediate photocoagulation of avascular retina was done in left eye while right eye was kept under observation. No further treatment was administered to either eye during follow up. Right eye showed gradual spontaneous ROP regression (Figure 3A). At 3 weeks following laser, the extra retinal fibrovascular proliferation in left eye regressed and plus disease also subsided (Figure 3B). At 6 months of follow up both eyes had regressed ROP.
Discussion
IFC and ROP are two different entities with completely different etiopathology and clinical manifestations. While IFC is a congenital disorder due to defective embryogenesis, ROP is an acquired disorder occurring in premature infants after birth following arrest of normal retinal vasculogenesis (4,5). While IFC occurs in the first trimester itself during the period of organogenesis, vascularization of the retina does not start until the 16th week of gestation and completes only at one month post birth (6). While ROP typically affects the peripheral retinal vasculature, IFC affects majorly the posterior outer layers of retina only in the region of the coloboma. Hence a direct causative association between the two conditions is highly improbable.
In our case, there was a striking asymmetry in the disease severity between two eyes, such that one eye required urgent treatment, while the other regressed spontaneously. Also, considering the systemic course, severe ROP was expected in both the eyes. Asymmetry of ROP has been noted earlier with respect to disease presentation and progression between twins (7), but this unusual inter eye asymmetry in IFC has not been reported till now. The eye having coexisting IFC manifested with less severe disease. The protective effect of IFC can be explained on the basis of differential production of proangiogenic factors between two eyes. The eye with IFC is expected to produce less angiogenic factors owing to lesser avascular retina, and this maybe proportional to the area involved. Fundal colobomas may lead to complete loss of choroid and outer retinal tissue over the involved area with only intercalary membrane (undifferentiated inner retina) and sclera left intact (8). The undifferentiated retina is less likely to produce proangiogenic factors as well.
Inter eye asymmetry in terms of severity of retinal vasculopathy has also been seen in other vasoproliferative disorders due to differential balance between proangiogenic and antiangiogenic factors. Recently, such asymmetry has been documented in a case of proliferative diabetic retinopathy with preexisting IFC, with less severe retinopathy noted in the eye with larger coloboma (9), hence substantiating our conjecture.
Conclusions
Thus it is possible that IFC, albeit damaging in its own respect, may be protective against disease progression in ROP. However, follow up should be done for complications related to the IFC itself.
Acknowledgments
Funding: None.
Footnote
Conflicts of Interest: All authors have completed the ICMJE uniform disclosure form (available at http://dx.doi.org/10.21037/aes.2017.12.07). The authors have no conflicts of interest to declare.
Ethical Statement: The authors are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee(s) and with the Helsinki Declaration (as revised in 2013). Informed written consent was obtained for all the procedures involved in management.
Open Access Statement: This is an Open Access article distributed in accordance with the Creative Commons Attribution-NonCommercial-NoDerivs 4.0 International License (CC BY-NC-ND 4.0), which permits the non-commercial replication and distribution of the article with the strict proviso that no changes or edits are made and the original work is properly cited (including links to both the formal publication through the relevant DOI and the license). See: https://creativecommons.org/licenses/by-nc-nd/4.0/.
References
- Jakobiec FA. Ocular Anatomy Embryology and Teratology. Philadelphia: Harper & Row, 1982:1027,1052-7.
- Onwochei BC, Simon JW, Bateman JB, et al. Ocular colobomata. Surv Ophthalmol 2000;45:175-94. [Crossref] [PubMed]
- Nakamura KM, Diehl NN, Mohney BG. Incidence, ocular findings, and systemic associations of ocular coloboma: a population-based study. Arch Ophthalmol. 2011;129:69-74. [Crossref] [PubMed]
- Good WVEarly Treatment for Retinopathy of Prematurity Cooperative Group. Final results of the Early Treatment for Retinopathy of Prematurity (ETROP) randomized trial. Trans Am Ophthalmol Soc 2004;102:233-48; discussion 248-50. [PubMed]
- Chang L, Blain D, Bertuzzi S, et al. Uveal coloboma: clinical and basic science update. Curr Opin Ophthalmol 2006;17:447-70. [Crossref] [PubMed]
- Mintz-Hittner HA, Kennedy KA, Chuang AZ, et al. Efficacy of intravitreal bevacizumab for stage 3+ retinopathy of prematurity. N Engl J Med 2011;364:603-15. [Crossref] [PubMed]
- Azad R, Chandra P, Patwardhan SD, et al. Profile of asymmetrical retinopathy of prematurity in twins. Indian J Ophthalmol 2010;58:209-11. [Crossref] [PubMed]
- Uhumwangho OM, Jalali S. Chorioretinal coloboma in a paediatric population. Eye (Lond) 2014;28:728-33. [Crossref] [PubMed]
- Moriya T, Ochi R, Imagawa Y, et al. A Case of Uveal Colobomas Showing Marked Left-Right Difference in Diabetic Retinopathy. Case Rep Ophthalmol 2016;7:167-73. [Crossref] [PubMed]
Cite this article as: Gangwe AB, Chandra P, Takkar B, Azad SV, Azad R. Iridofundal colobomas may lower severity of retinopathy of prematurity. Ann Eye Sci 2018;3:10.


